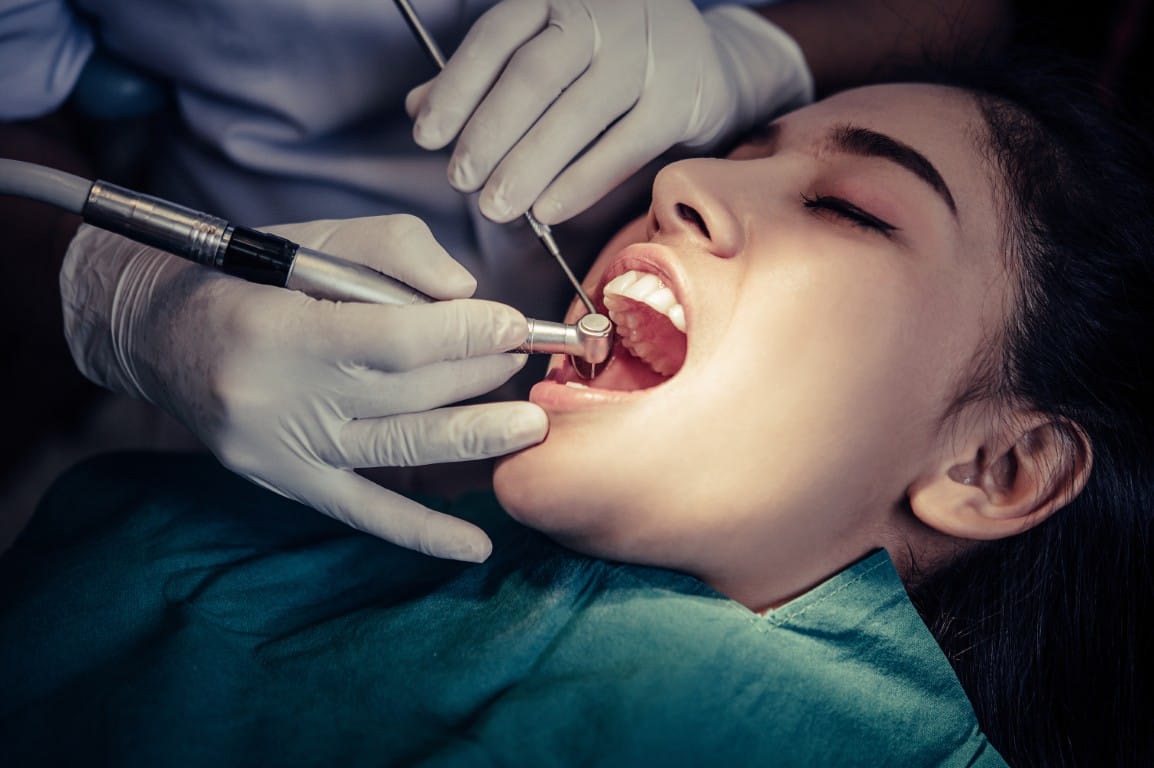
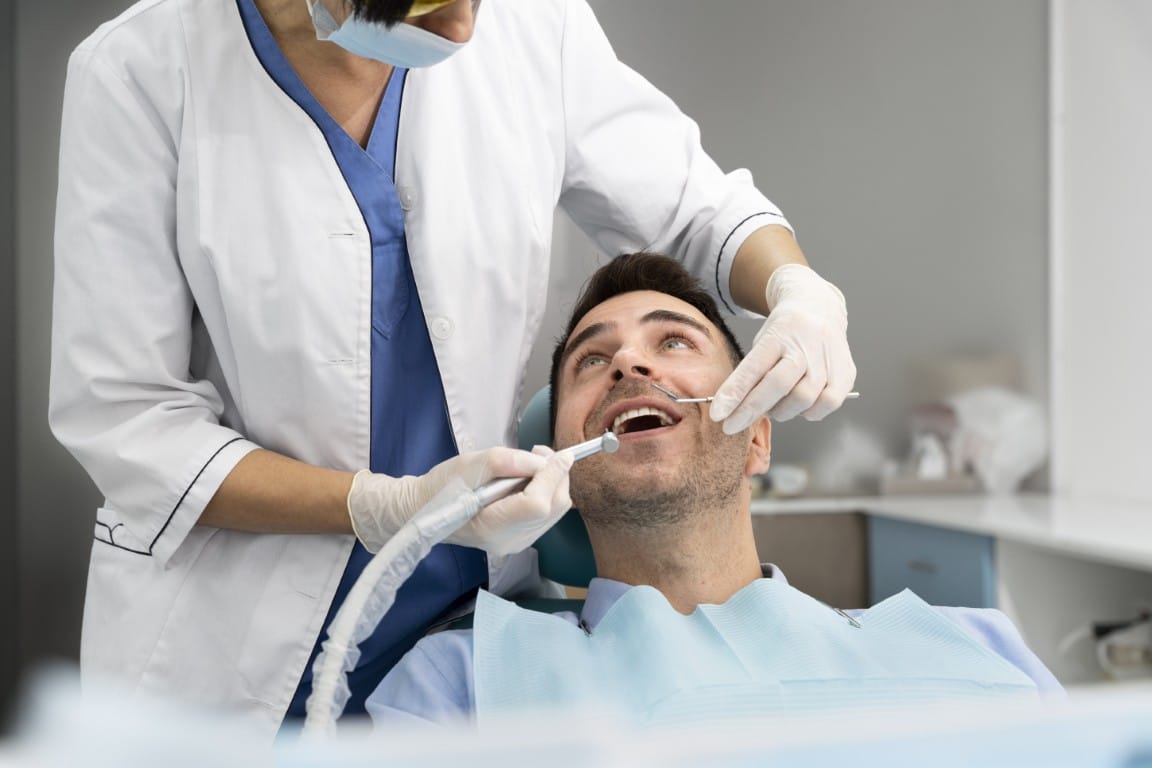
If you're living with an autoimmune disease, you're probably managing a complex set of symptoms and treatments. What many patients don't realize is that autoimmune conditions can have a significant impact on your teeth and gums — sometimes before other symptoms even appear.
Understanding the connection between autoimmune diseases and oral health can help you stay ahead of problems and protect your smile.
How Autoimmune Diseases Affect Your Mouth
In autoimmune diseases, the immune system mistakenly attacks healthy tissue. When this affects the mouth, it can lead to:
- Chronic dry mouth — reduced saliva production leaves teeth vulnerable to decay
- Increased gum disease risk — inflammation throughout the body extends to the gums
- Mouth sores and ulcers — painful lesions that interfere with eating and oral hygiene
- Accelerated tooth decay — multiple factors combine to damage teeth faster than normal
- Jaw problems — joint inflammation can affect the TMJ
Specific Autoimmune Conditions and Oral Health
Sjogren's Syndrome
Sjogren's syndrome directly targets the salivary glands, dramatically reducing saliva production. This is perhaps the autoimmune condition most devastating to oral health because saliva is your teeth's primary defense against decay. Without adequate saliva:
- Bacteria multiply rapidly
- Food particles aren't washed away
- Acid from food and bacteria isn't neutralized
- Cavity rates can increase dramatically — some patients develop multiple new cavities every few months
Lupus (Systemic Lupus Erythematosus)
Lupus can cause oral ulcers that appear on the palate, cheeks, and gums. These sores can be painful and may flare up during disease activity. Lupus also increases susceptibility to gum disease and can affect jaw joints. Some lupus medications further complicate dental care by suppressing the immune system or causing dry mouth.
Rheumatoid Arthritis (RA)
Research has revealed a strong bidirectional relationship between RA and periodontal disease. The same inflammatory processes that attack joints can attack gum tissue. Additionally, RA can affect the TMJ (jaw joint), causing pain, stiffness, and difficulty opening the mouth — which in turn makes dental care more challenging.
Crohn's Disease and Inflammatory Bowel Disease
These conditions can cause oral symptoms including mouth ulcers, swollen gums, and cobblestone-like mucosal changes. Nutritional deficiencies common in IBD patients (particularly vitamin B12, iron, and folate) can also affect oral health.
Type 1 Diabetes
Type 1 diabetes (an autoimmune form of diabetes) significantly increases the risk of gum disease. High blood sugar feeds oral bacteria and impairs the body's ability to fight gum infections. The relationship works both ways — severe gum disease can make blood sugar harder to control.
Celiac Disease
Celiac disease can cause enamel defects — pitting, discoloration, and bands of missing enamel on permanent teeth. These defects develop during childhood when teeth are forming. Canker sores are also common in celiac patients.
Medications and Their Dental Side Effects
Many medications used to treat autoimmune conditions have oral side effects:
- Immunosuppressants (methotrexate, azathioprine) — increase risk of oral infections and slow healing after dental procedures
- Corticosteroids (prednisone) — can promote oral candidiasis (thrush) and bone loss in the jaw
- Biologics (Humira, Enbrel) — suppress immune function, increasing infection risk
- NSAIDs — long-term use can contribute to dry mouth
Always inform your dentist about all medications you're taking so your dental care can be coordinated accordingly.
Protecting Your Teeth with an Autoimmune Condition
Autoimmune patients need a more proactive approach to dental care:
- More frequent dental visits: Every 3-4 months instead of the standard 6 months, especially for Sjogren's patients
- Prescription fluoride toothpaste: Higher-concentration fluoride can help protect teeth when saliva is reduced
- Saliva substitutes and stimulants: Products like Biotene or prescription medications (pilocarpine) can help manage dry mouth
- Sugar-free gum: Chewing stimulates saliva production — look for xylitol-containing gum, which also inhibits cavity-causing bacteria
- Gentle oral hygiene tools: Soft toothbrushes, alcohol-free mouthwash, and waxed floss are kinder to sensitive mouths
- Coordinate care: Your dentist and rheumatologist (or other specialist) should communicate about your treatment plan
Specialized Dental Care in Berkeley
At Acorn Family Dental Care, Dr. Teah Nguyen understands the unique dental challenges that autoimmune patients face. We provide personalized treatment plans that account for your medications, symptoms, and overall health picture.
If you have an autoimmune condition and want to ensure your dental care is properly managed, contact our Berkeley office to schedule an appointment.