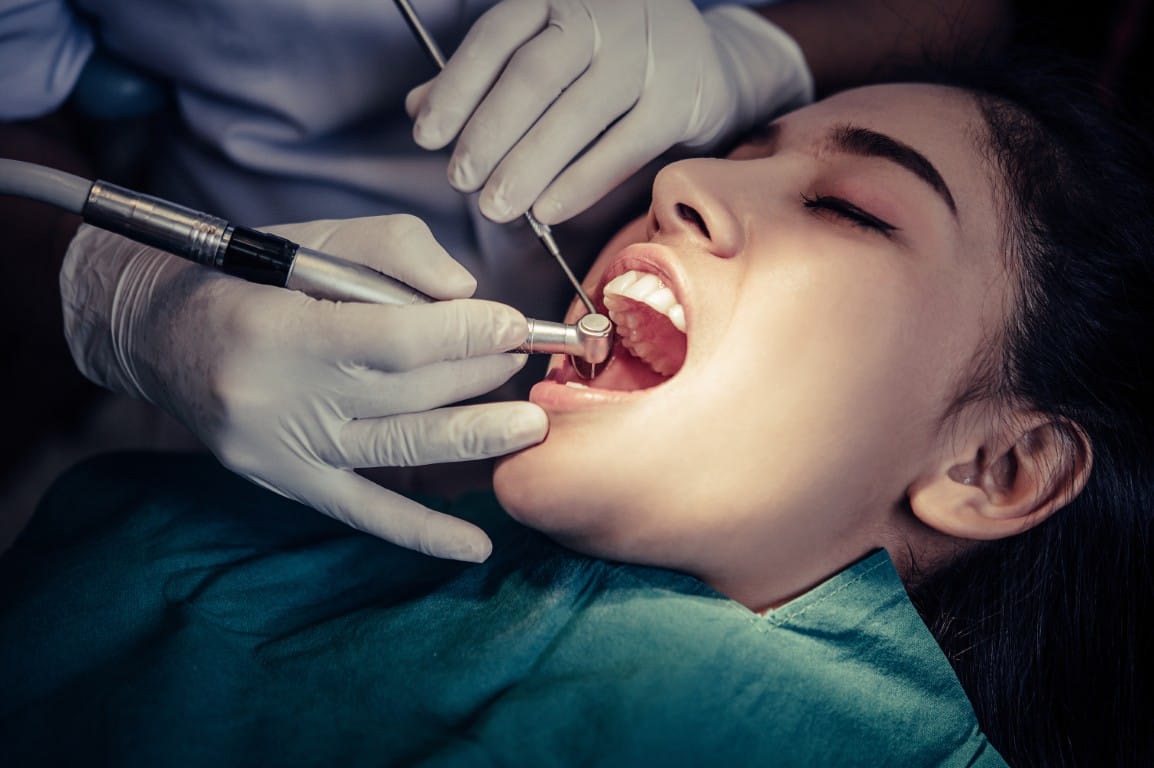
If your gums bleed when you brush, your breath has a metallic edge that won't quit, or your teeth suddenly feel longer than they used to — those are early signs of gum disease, and they matter more than most people realize. Nearly half of American adults over 30 have some form of periodontal disease, according to the CDC's oral health surveillance data. Most don't know it until a dentist points it out.
The good news: caught at the gingivitis stage, gum disease is fully reversible. Caught at periodontitis, it's manageable but the bone loss is permanent. The window between the two stages is the most important one in your mouth — and the symptoms that mark it are easy to spot once you know what to look for. At Acorn Family Dental Care in Berkeley, Dr. Teah Nguyen sees the full range every week, from a teenager with bleeding gums to a long-time patient catching their first hint of bone loss. The earlier you act, the less treatment you need.
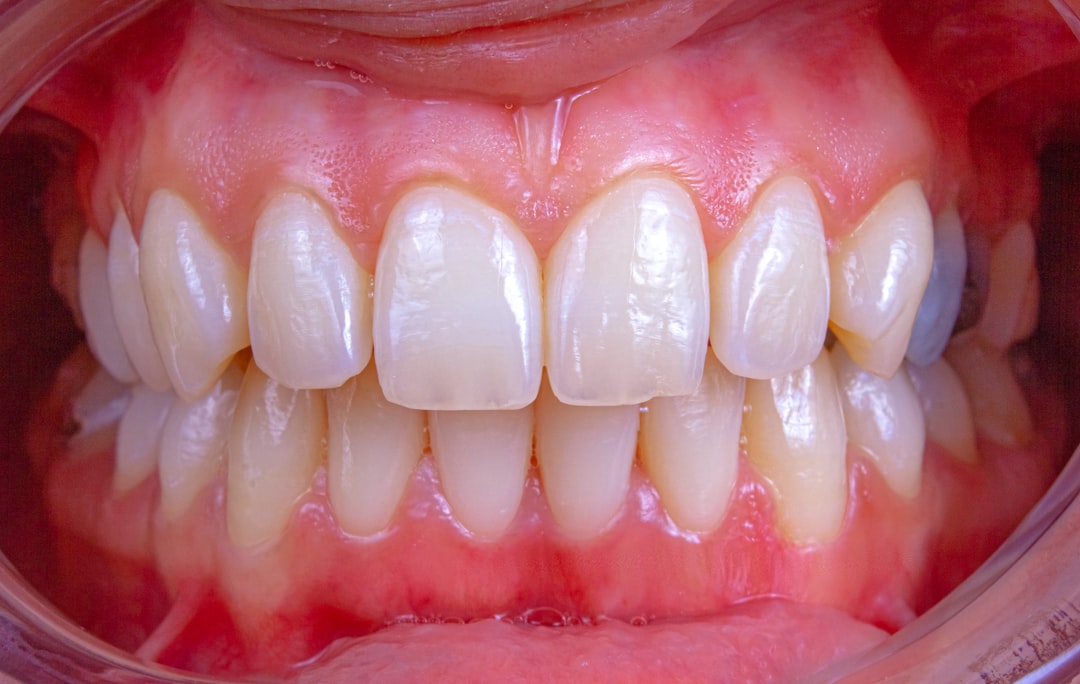
Gingivitis vs. Periodontitis: The Two Stages of Gum Disease
Gum disease isn't one condition — it's a spectrum, and where you sit on it changes everything about treatment.
Gingivitis is the early stage. Plaque sits along the gumline, the bacteria release toxins, and your gums respond with inflammation. Tissue gets red, puffy, and bleeds easily. Nothing structural has been damaged yet. A professional cleaning plus a tightened-up home routine will reverse it within a few weeks.
Periodontitis is what gingivitis becomes if it's left alone. The inflammation moves below the gumline, your body's immune response starts breaking down the ligaments and bone that hold teeth in place, and pockets form between the gum and the tooth where bacteria multiply. Once bone is lost, it doesn't grow back. Treatment shifts from a regular cleaning to scaling and root planing — and in advanced cases, gum surgery.
Why Early Detection Changes Everything
The hardest thing about gum disease is that it rarely hurts in the early stages. There's no toothache to push you into the chair — just slow, quiet inflammation you can talk yourself out of noticing. By the time discomfort shows up, you're often already in periodontitis territory. That's why every routine cleaning at our office includes pocket-depth measurements: 1–3 mm is healthy, 4 mm is the watch zone, and 5+ mm is active disease. Numbers catch the shift before symptoms do.
8 Early Warning Signs You Might Have Gum Disease
One of these symptoms in isolation isn't a diagnosis — but two or more, especially if they're getting worse, is your cue to book an exam. Here are the early signs of gum disease patients describe most often when they finally come in.

1. Bleeding Gums When You Brush or Floss
This is the single most reliable early indicator. Healthy gums do not bleed during normal brushing or flossing — not even when you've been a little vigorous. The pink in your sink is your immune system responding to bacterial toxins along the gumline. If it happens once after a popcorn injury, fine. If it's happening multiple times a week, it's gingivitis until proven otherwise. Bleeding gums causes are almost always inflammatory, not mechanical.
2. Red, Swollen, or Puffy Gum Tissue
Healthy gums are pale pink, firm, and stippled like an orange peel. Gums that look bright red, shiny, or puffy along the edges of the teeth are inflamed. The change is often gradual enough that you don't notice it on yourself — that's why it's worth glancing at the gumline in good light every couple of weeks, especially right after you brush.
3. Gums That Are Pulling Away from Your Teeth
If your teeth look longer than they used to, or you can suddenly see a sliver of root above the gumline, your gums are receding. Recession can come from aggressive brushing, but in adults over 35 it's usually a sign of underlying periodontal disease pulling the tissue down. The exposed root is also more sensitive to cold and more vulnerable to decay.
4. Persistent Bad Breath That Won't Clear Up
Brushing, flossing, and mouthwash should knock out most bad breath in under a minute. Halitosis that returns within an hour — or never fully clears — is often coming from the bacterial colonies thriving in deep gum pockets, where your toothbrush can't reach. Our guide on how to eliminate bad breath permanently covers the full diagnostic path, but if your gums are also bleeding, periodontal disease is the first place to look.
5. Teeth That Feel Loose or Are Shifting
Adult teeth shouldn't move. If a front tooth feels slightly loose when you press your tongue against it, or if your bottom teeth have started crowding more noticeably, the bone supporting them is being lost. This is a periodontitis-stage sign — not gingivitis — and it's the point at which treatment urgency goes way up.
6. Pain or Discomfort When Chewing
Sore gums while eating, especially with crusty bread or a tough piece of meat, suggests the supporting tissue is inflamed. Patients usually describe it as "tender" rather than the sharp pain of a cracked tooth or cavity. The tenderness tends to center around one or two teeth where the pocketing is deepest.
7. Pus Along the Gumline
A small amount of cloudy fluid expressed when you press the gum near a tooth is pus — your body's response to active bacterial infection. It might appear as a faint white seam at the edge of the gum, or a bad taste that returns after rinsing. This is an unambiguous sign of advanced disease and warrants an exam within the week.
8. Changes in How Your Bite Fits Together
If your teeth meet differently than they did six months ago — your night guard suddenly fits poorly, or one side feels like it's hitting first — bone loss may be allowing teeth to shift positions. Bite changes in adults are almost never random. They're the structural consequence of either periodontal bone loss, a cracked tooth, or worn-out restorations.
Who Is at Highest Risk for Gum Disease?
Gum disease isn't purely about how well you brush. Two patients with identical home routines can have wildly different outcomes because of what's going on systemically.
Diabetes, Smoking, Hormonal Changes, and Genetics
- Diabetes. Elevated blood sugar feeds the bacteria responsible for gum disease and slows healing. Patients with poorly controlled type 2 diabetes are roughly three times more likely to develop severe periodontitis.
- Smoking and vaping. Nicotine constricts blood flow to the gums, masking the bleeding that would normally signal inflammation. Smokers often have advanced disease without ever seeing pink in the sink.
- Hormonal shifts. Pregnancy, perimenopause, and the start or end of hormonal birth control all change how gum tissue responds to bacteria. "Pregnancy gingivitis" is its own well-documented pattern.
- Genetics. Roughly 30% of the population is genetically more susceptible to aggressive periodontitis regardless of hygiene. If a parent lost teeth to gum disease, your risk is materially higher.
- Autoimmune conditions. Lupus, rheumatoid arthritis, and Sjögren's syndrome all alter the immune response in the mouth. Our guide on protecting teeth and gums when you have an autoimmune condition walks through the specific risks.
- Stress and poor sleep. Both raise systemic inflammation and reduce the immune response that holds bacteria in check.
How Gum Disease Affects Your Overall Health
The mouth isn't a sealed compartment. The same bacteria that drive periodontal pockets travel through the bloodstream, and the inflammation gum disease creates is measurable elsewhere in the body.
The Link to Heart Disease, Diabetes, and Systemic Inflammation
Research from the National Institute of Dental and Craniofacial Research and decades of follow-up studies have linked periodontal disease to higher rates of cardiovascular events, harder-to-control blood sugar in diabetics, complications during pregnancy, and even respiratory infections in older adults. The relationship runs both directions — diabetes makes gum disease worse, and gum disease makes diabetes harder to control.
None of this means gum disease causes heart disease. It means the chronic inflammation and bacterial load you carry in an untreated mouth contribute to the inflammatory burden the rest of your body has to manage. Our deeper post on how periodontal disease connects to your general health walks through the latest research in detail.
How Gum Disease Is Treated
Treatment depends almost entirely on which stage we catch the disease at. The earlier the stage, the less invasive — and less expensive — the path forward. Our approach to gum disease treatment in Berkeley is staged to match the severity, never to over-treat.
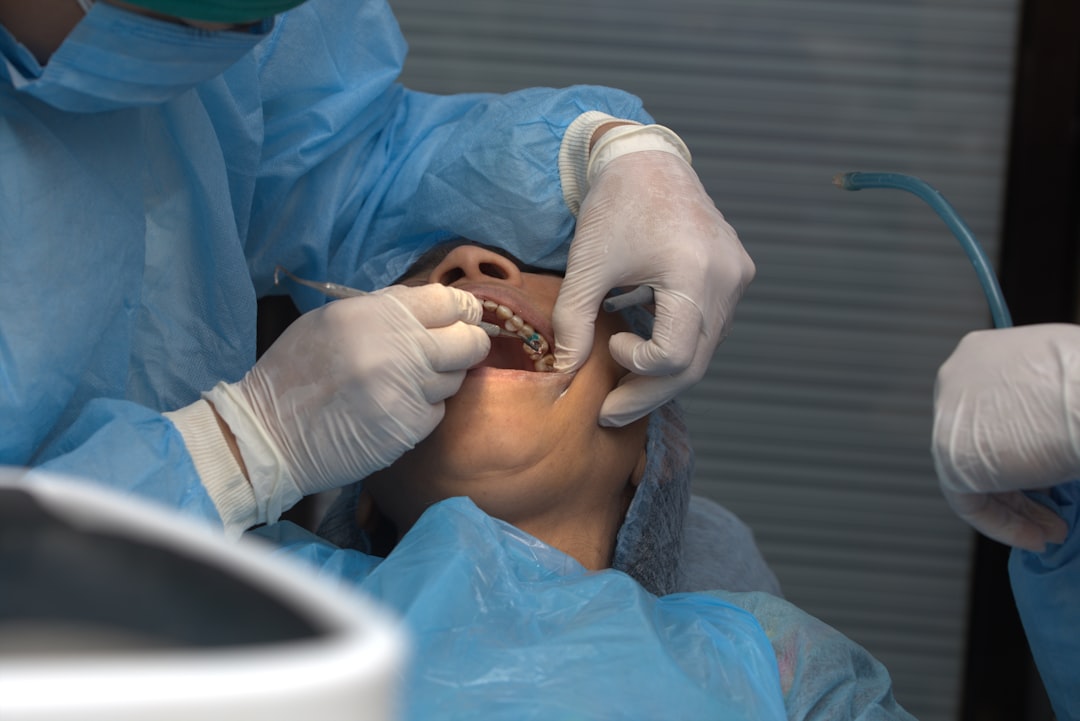
Stage 1: Professional Cleaning and Improved Home Care
Gingivitis usually clears within two to four weeks of a thorough professional cleaning combined with consistent home care — twice-daily brushing with a soft-bristled brush, daily flossing, and an antimicrobial rinse if we recommend one. Most patients see the bleeding stop within a week. We confirm the gums have fully healed at your next checkup. The full breakdown of what happens at this visit lives on our page about the benefits of professional dental cleanings.
Stage 2: Scaling and Root Planing (Deep Cleaning)
Once disease has crossed into early periodontitis, a regular cleaning isn't enough. Scaling and root planing — sometimes called a "deep cleaning" — uses ultrasonic and hand instruments to remove tartar from below the gumline and smooth the root surfaces so the gum tissue can reattach. We typically split it into two appointments, treat under local anesthesia, and follow up at 6–8 weeks to confirm the pockets have shallowed.
Stage 3: Surgical Treatment for Advanced Disease
For patients who arrive with deep pocketing, significant bone loss, or pockets that don't respond to scaling, surgical options become necessary. These can include flap surgery to access and clean root surfaces directly, bone grafting to rebuild lost support, or guided tissue regeneration. Surgery isn't the first move — it's reserved for cases where conservative treatment can't reach the disease. When it is needed, it stops the progression and gives the rest of the dentition a longer runway.
What You Can Do at Home to Prevent Gum Disease
Prevention is unglamorous but reliable. The patients who never need scaling and root planing all do roughly the same things:
- Brush twice daily for two minutes with a soft-bristled brush angled at 45 degrees toward the gumline — not horizontally across the teeth.
- Floss every day, or use a water flosser if traditional floss is hard for you. The point is to disrupt the plaque between teeth before it hardens into tartar.
- Get a professional cleaning every six months — every three months if you've already had periodontal treatment. Our post on why routine checkups stop tartar before it starts covers exactly what gets removed at each visit.
- Don't smoke or vape. If you've been thinking about quitting, gum health is one of the fastest visible rewards — bleeding usually decreases within weeks.
- Manage diabetes and stress. Stable blood sugar and lower cortisol levels both protect the gums.
- Watch your gums in the mirror. Once a month, in good light, look at the line where each tooth meets the gum. You'll catch changes earlier than your dentist will.
Bleeding gums or breath that won't clear up?
A periodontal exam takes 30 minutes and tells us exactly which stage you're in. Schedule online or call Acorn Family Dental Care — Dr. Nguyen will measure pocket depths, take any X-rays needed, and walk you through your options before any treatment is recommended.
Call (510) 848-0114If you've been putting off a cleaning because nothing actively hurts, that's the most common — and most expensive — mistake patients make with gum disease. Catching gingivitis costs the price of a hygiene visit. Catching periodontitis at year three costs scaling, root planing, possibly surgery, and the bone you've already lost. The disease moves slowly, but it doesn't reverse itself once it crosses the line. The cheapest, easiest version of treatment is the one you book this month.
Frequently Asked Questions
What are the very first signs of gum disease?
The earliest sign of gum disease is almost always bleeding when you brush or floss. That's gingivitis. It usually shows up before any pain — gums look slightly red or puffy along the edge of the tooth, and they bleed easily. At this stage the disease is fully reversible with a professional cleaning and better home care.
Can gum disease go away on its own?
Gingivitis — the earliest stage — can be reversed with consistent brushing, flossing, and a professional cleaning to remove the hardened plaque your toothbrush can't reach. Once gum disease progresses to periodontitis, the bone loss is permanent. The disease can be stopped and managed, but the tissue you've already lost doesn't grow back.
How fast does gum disease get worse?
It varies widely. Some patients move from healthy gums to gingivitis in weeks of poor oral hygiene. The progression to periodontitis usually takes months to years and depends on genetics, smoking, diabetes control, and how often you see a hygienist. Smokers and uncontrolled diabetics tend to progress fastest.
Do bleeding gums always mean gum disease?
Almost always, yes. Healthy gums don't bleed during normal brushing or flossing — even when you've been a little aggressive. Occasional bleeding from a single spot after a popcorn injury is different from gums that bleed routinely. If you're seeing pink in the sink most days, that's gingivitis until proven otherwise.
What's the best gum disease treatment in Berkeley?
For gingivitis, a thorough professional cleaning followed by a daily home routine of brushing twice and flossing once usually clears it within a few weeks. For periodontitis, scaling and root planing — a deeper cleaning below the gumline — is the standard first step. At Acorn Family Dental Care we measure pocket depths at every checkup so we catch the shift between the two stages early.
Is gum disease contagious?
The bacteria that cause gum disease can be transferred between people through saliva — sharing utensils, kissing, or a parent tasting a child's food. Whether the bacteria actually take hold and cause disease depends on the other person's immune response and oral hygiene. So it's not contagious in the way a cold is, but the bacteria do spread.
Photos by Ozkan Guner, Konstantinos Papadopoulos, Rosario Fernandes, and Shedrack Salami on Unsplash.